Colorectal cancers start as polyps. Over time, the cells in these polyps can undergo genetic changes, causing the cells to multiply uncontrollably, leading to cancer.
How quickly do colon polyps grow before they become cancerous? The growth rate varies significantly depending on the type of polyp and individual factors. Generally, they grow slowly over several years.
This article further explores the factors influencing how fast polyps grow in the colon, the factors influencing their growth, and ways to prevent colorectal cancer.
Table of Contents
ToggleIt Takes 10 Years For Colon Polyps To Grow
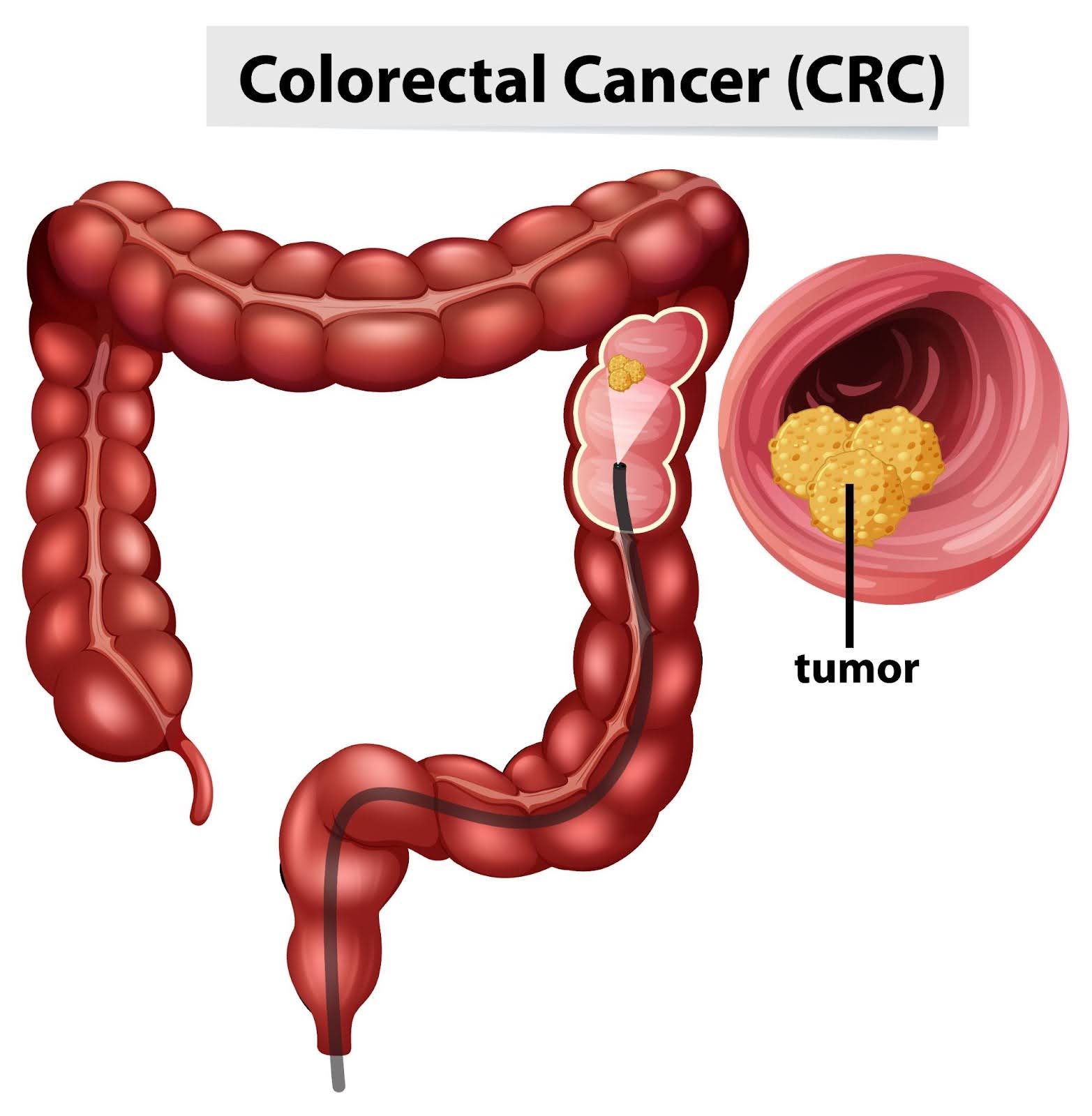
It can take about 10 years for a small colon polyp to develop into colorectal cancer, although this timeline can vary. According to a study, colonic polyps can invade the colonic wall and degenerate into cancer between 5 to 15 years.
The growth rate can be affected by the type of polyp, genetics, diet, lifestyle, and the presence of conditions like familial adenomatous polyposis (FAP) or Lynch syndrome, which can lead to a faster development of polyps and a higher risk of colon cancer.
So, even though it can take a decade for polyps to grow, this doesn’t mean you should wait or forget about getting checked for colorectal cancer. It’s a big reason why you should get a colonoscopy regularly.
Types Of Colon Polyps
A colonoscopy is a key screening tool used to identify and remove colon polyps. The doctor will classify the colon polyps found in the large intestine into two types: adenomatous and hyperplastic.
Adenomatous Polyps (Adenomas)
These are considered pre-cancerous and are the type most associated with developing colon cancer. They can take many years to develop into cancer, typically 10 to 15 years. Adenomatous polyps, particularly those larger than 1 cm or with more villous features, are more likely to become cancerous.
Hyperplastic Polyps and Inflammatory Polyps
These are generally not considered pre-cancerous. They are more common and usually don’t carry the same risk of developing cancer as adenomas do. Their growth rate is similar to that of adenomas, but they are less likely to develop cancer.
Other Factors That Can Influence The Polyps Growth Rate
In addition to the type of colon polyps, many other factors can affect their growth and their potential to become cancerous.
-
- Size of Polyp: Polyps larger than 1 cm have a significantly increased risk of containing cancerous cells. According to the American Cancer Society, the likelihood of a larger polyp being cancerous is higher than that of a smaller polyp.
-
- Number of Polyps: Individuals with multiple polyps, a condition known as polyposis, have a higher risk for colorectal cancer. Research indicates that the number of polyps correlates with the risk of colorectal cancer.
-
- Genetic Factors: Conditions like familial adenomatous polyposis (FAP) and Lynch syndrome are associated with a higher risk and more rapid growth of polyps. FAP, for example, leads to hundreds to thousands of polyps at a young age and nearly a 100% risk of colorectal cancer if not managed.
-
- Age: Polyp prevalence increases with age. Studies have shown that the incidence of adenomas increases significantly in individuals over 50 years of age, which is why colon cancer screening recommendations often start at this age.
-
- Diet and Lifestyle: Diets high in red and processed meats and low in fibre, fruits, and vegetables are linked with an increased risk of colorectal cancer. Obesity, smoking, and physical inactivity are also risk factors. A study in the “Journal of Nutrition” highlighted the role of diet in polyp development.
-
- Ethnicity and Race: African Americans are at a higher risk for colorectal cancer and may develop polyps at a younger age. This disparity suggests a potential difference in polyp growth rates among different ethnic groups, as noted in the American Journal of Gastroenterology research.
-
- Inflammatory Bowel Disease: Chronic inflammation from conditions like ulcerative colitis or Crohn’s disease is associated with Dysplasia and an increased risk of colorectal cancer. Studies in the “Gastroenterology” journal have shown that the risk of cancer increases the longer a person has inflammatory bowel disease.
-
- Previous Polyp History: A history of adenomas, especially advanced adenomas, is a decisive risk factor for the development of subsequent adenomas or colorectal cancer. The risk increases with the number and size of previously removed polyps, as indicated in studies.
-
- Family History: A family history of polyps or colorectal cancer increases the risk. Studies suggest that first-degree relatives of patients with colon cancer or adenomatous polyps have a two to three times higher risk of developing colorectal cancer or polyps themselves.
Screening And Diagnostic Procedures For Colon Polyps
Most polyps do not turn into cancer. However, removing them and analysing them is a key step in preventing colorectal cancer. Regular colorectal cancer screening, especially for individuals at higher risk (due to age, family history, genetic factors, etc.), is crucial for early detection and effective management.
Doctors use a combination of screening methods and diagnostic procedures to determine if colon polyps are cancerous. The process typically involves the following steps:
-
- Colonoscopy: This is the most common and effective method for detecting colon polyps using a colonoscope. If polyps are found in the colon, they can often be removed during the procedure.
-
- Polyp Removal: Polyps found during a colonoscopy are usually removed using tools passed through the colonoscope. This is important not only for diagnosis but also for prevention, as removing polyps can prevent them from turning into cancer.
-
- Histopathological Examination: The removed polyps are then sent to a laboratory for histopathological examination to identify their type and check for cancer signs.
-
- Assessing Dysplasia: The pathologist looks for Dysplasia. As mentioned, Dysplasia is a pre-cancerous condition, and its presence in a polyp is a strong indicator of potential for developing into cancer.
-
- Genetic Testing of the Polyp: Sometimes, genetic testing is performed on the polyp tissue to identify specific genetic mutations. This can help in assessing the risk of colorectal cancer and in guiding treatment decisions, particularly in hereditary cancer syndromes.
- Follow-Up Surveillance: Doctors will recommend a follow-up schedule for future colorectal screenings after polyps are removed and analysed. The frequency of follow-up colonoscopies depends on the number, size, and type of polyps and whether they contain cancer cells.
What Happens If Colon Polyps Are Cancerous
If colon polyps are found to be cancerous, the course of action and treatment will depend on various factors, including the cancer stage, the polyp’s size and location, and the patient’s overall health. Here’s a general outline of what might happen:
-
- Staging the Cancer: The next step is determining the cancer stage if a polyp is found to be cancerous. This involves assessing how deeply the cancer has penetrated the colon or rectum wall and whether it has spread to other parts of the body. Staging may involve additional tests like CT scans, MRIs, or ultrasounds.
-
- Surgical Intervention: Surgery is a standard treatment for colorectal cancer. Removing the polyp during the colonoscopy might be sufficient if the cancer is in its early stages and confined to the polyp. For larger cancers, more extensive surgery may be needed to remove the part of the colon or rectum where the cancer is located.
-
- Additional Treatments: If the cancer is more advanced or if there’s a higher risk of it coming back, additional treatments might be necessary. Depending on the colon cancer stage, the treatment can include chemotherapy, radiation therapy, or targeted therapy.
- Follow-up Care: After treatment, patients are required to do regular visits to the doctor and possibly additional colonoscopies or other tests to monitor for any signs of cancer returning or new polyps forming.
Ways To Prevent Colon Polyps From Becoming Colon Cancer

Aside from regular colon cancer screening, there are lifestyle changes that you can incorporate to stop colon polyps from growing or forming at all.
-
- Adopt a healthy diet: Eat more fruits, vegetables, whole grains, and legumes to boost fibre. Reduce red or processed meat like bacon and sausages as they are linked to an increased risk of colorectal cancer. You should also consume foods rich in calcium and vitamin D.
-
- Maintain a Healthy Weight: Obesity increases the risk of colon cancer and polyps. Aim for a healthy weight through diet and exercise for at least 30 minutes on most days of the week.
-
- Avoid Tobacco and Limit Alcohol: Smoking is a known risk factor for colorectal cancer and polyps. Quitting smoking can reduce this risk. You must also limit alcohol consumption.
-
- Consider Aspirin or Other Nonsteroidal Anti-inflammatory Drugs (NSAIDs): Some studies suggest that aspirin or other NSAIDs may help reduce the risk of polyps. However, these should only be taken under a doctor’s advice due to potential side effects.
Conclusion About How Fast Colon Polyps Grow
The growth rate of colon polyps can vary significantly, but generally, they develop over years rather than months. While not all polyps will turn into cancer, some can, especially if they’re left undetected and untreated. This slow growth rate highlights the importance of regular screenings so you can catch them earlier for better prognosis.
At Advanced Colorectal and General Surgery, we offer same-day colonoscopy. You will undergo consultation and screening all in the same day.
Our colorectal specialist will provide an in-depth diagnosis to help you understand your unique health needs and risks. Contact us to book a consultation today!
Frequently Asked Questions About How Fast Colon Polyps Grow
Do Colon Polyps Grow Back?
Yes, colon polyps can grow back, but it’s not inevitable. The likelihood of polyps reappearing depends on factors like the type of polyps initially removed, the number of polyps, and your genetic predisposition. People who have had polyps before are at a higher risk of developing new polyps in the future.
How Fast Do Colon Polyps Grow Back?
The growth rate of new polyps can vary. Typically, it takes several years for new polyps to develop and grow. The exact timeline can depend on individual factors like genetics, lifestyle, and certain medical conditions. Regular follow-up screenings, like colonoscopies, are recommended to monitor and manage this risk.
Do Colon Polyps Cause Constipation?
In most cases, small colon polyps do not cause symptoms and are usually not associated with constipation. However, larger polyps might cause bowel habit changes, including constipation. This is more common if the polyp partially obstructs the colon, though such large polyps are less common.
Is There Any Pain Associated With Colon Polyps?
Colon polyps themselves usually don’t cause pain. If a polyp grows large enough to cause obstruction or significant irritation in the colon, there might be discomfort or pain, but this is relatively rare.