Anal Fistulas & Perianal Abscess Removal In Singapore
Insurance
Our surgery is on the panel of most of the major insurance companies and if you are covered by corporate insurance, you may be entitled to a cashless visit to our clinic.
Get In Touch
Table of Contents
Introduction
Anal fistulas and perianal abscesses are painful and can be challenging to treat. It is also known as a common complication of inflammatory bowel disease (IBD). It is a recurrent infection that causes discomfort and disability to the sufferer. And it can be highly uncomfortable and disrupt daily activities.
You might be worried about the cost of abscess removal in Singapore but waiting too long can lead to more severe problems, like the spread of bacterial infection or the pus build-up causing the skin to swell. And unlike other diseases or illnesses, antibiotics are not very effective in treating perianal abscesses.
If you have an abscess that needs treatment, it’s essential to see a specialist for perianal abscess removal in Singapore right away.
What Are Perianal Abscesses?
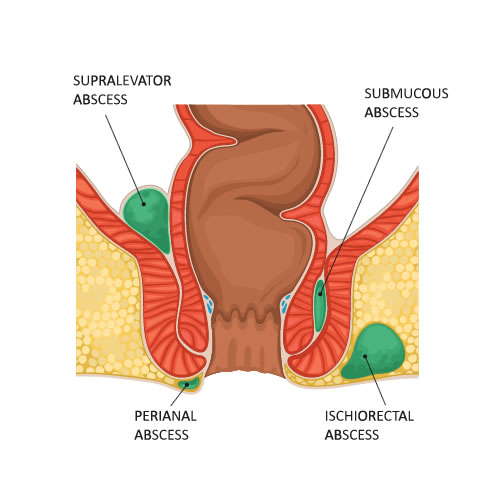
The inside of our anuses contains numerous glands that produce fluid. Sometimes, these glands get blocked or clogged, causing a build-up of bacteria. Over time, this can swell up and result in the tissue around the area becoming infected and filled with liquid. This is also known as an anal abscess.
They are typically caused by bacterial infections from perianal abscesses or other factors introducing bacteria into the anal glands or surrounding tissues.
Generally, doctors recommend Singaporeans undergo an anal abscess removal in Singapore to prevent further complications and infections.
What Is An Anal Fistula?

Wondering what causes an anal fistula to develop? This condition stems from untreated perianal abscess. When a perianal abscess is not properly drained or if the infection persists, it can lead to the formation of a fistula.
The infection tracks through the surrounding tissues, creating a tunnel that connects the infected area to the outside of the body. This tunnel allows for the continuous drainage of fluids and can result in chronic symptoms. Other less common causes of anal fistulas include Crohn’s disease, diverticular disease, TB and HIV.
Anal fistulas can cause unpleasant symptoms, and will not usually get better on their own. Surgery is recommended in almost all cases.
Prevention is better than cure. Hence it is important to seek timely perianal abscess surgery in Singapore to reduce both infection and the risk of anal fistulas developing.
What Are The Symptoms Of Anal Fistulas And Perianal Abscess
An anal abscess is common among active adults from 30 to 50 years old. It usually causes the skin condition to worsen, causing discomfort around the anus. Some of the common symptoms are:
- Skin irritation around the anus
- A constant, throbbing pain that may be worse when you move around
- Smelly discharge from near your anus
- Passing pus or blood when you pass motion.
- A “pimple” near the anus that does not go away.
- Swelling and redness around your anus and a high temperature (fever) if you also have an abscess
For anal fistulas, the signs can vary depending on the specific characteristics of the fistula and its location. Common symptoms associated with anal fistulas may include:
- Ongoing anal discomfort or pain ranging from mild to severe
- Continuous or intermittent drainage of pus, mucus, blood, or clear fluid
- Noticeable swelling or a lump near the anus or in the perianal area
- Itching and irritation of the surrounding skin
- Recurrent infections cause increased pain, swelling, warmth, redness, and fever
- Discomfort during bowel movements
- Bloody stool or blood in drainage
If you are worried or unsure of your current condition, do not hesitate to contact us to make an appointment and find out more about abscess removal or anal fistula surgery costs in Singapore.
Dr QM Leong is one of the experienced colorectal surgeons and has handled many cases of colorectal surgery, anal abscess and will be able to provide accurate diagnosis and proper treatment for abscess removal in Singapore.
Common Investigations For Anal Fistulas And Perianal Abscess
After a thorough history and physical examination which includes a rectal examination and proctoscopy, further tests such as a colonoscopy and MRI scan may be required.
The reason for the colonoscopy is to exclude TB, diverticular disease and Crohn’s disease. An MRI scan may be essential to evaluate the anatomy of the fistula tract.
If the tract extends higher into the rectum and it involves the anal sphincter muscles, surgery can become more complicated.
Healthcare professionals may employ various diagnostic tools to determine the best course of treatment. These may include a physical examination of the perianal area, a digital rectal exam to assess the anal canal and imaging studies such as a CT scan to visualise the fistula tract and identify any associated abscesses.
How Are Anal Fistulas And Perianal Abscess Treated
Treatment of fistulas and abscesses is surgery as these conditions do not resolve with medication (antibiotics) or on their own. There are several options and the correct surgery depends mainly on the type of fistula (simple vs complicated and high vs low fistulas).
Simple fistulas have a single opening internally and externally. Complicated fistulas may have multiple tracks with multiple openings (some involving muscle). Low fistulas have internal openings near the anus while high fistulas have internal openings deeper in the rectum, hence may involve sphincter muscle.
The aim of surgery is to heal the fistula while avoiding damage to the sphincter muscles, which could potentially result in loss of bowel control (bowel incontinence). Almost all surgery is done under general anaesthesia.
Here are the main options:
Fistulotomy
The most common type of surgery for anal fistulas is a fistulotomy. This involves cutting along the whole length of the fistula to open it up so it heals as a flat scar.
A fistulotomy is the most effective treatment for many anal fistulas, it is usually only suitable for low simple fistulas that do not pass through much of the sphincter muscles, as the risk of incontinence is lowest.
In cases where the risk of incontinence is considered too high, another procedure may be recommended instead.
Seton Techniques (Loose VS Cutting)
If your fistula passes through a significant portion of the anal sphincter muscle (high and complicated fistulas), the surgeon may initially recommend inserting a seton.
A seton is a piece of surgical thread that’s left in the fistula for several weeks to keep it open. This allows it to drain and helps it heal, while avoiding the need to cut the sphincter muscles.
Loose setons allow fistulas to drain, but do not cure them. To cure a fistula, tighter setons may be used to cut through the fistula slowly.
Hence the initial surgery may be to insert a loose seton to drain the infection, followed by a second surgery on a later date to convert the loose seton to a cutting seton.
Advancement Flap Procedure
An advancement flap procedure may be considered if your fistula passes through the anal sphincter muscles (high fistulas). This involves scraping out the fistula and covering the internal opening where it enters the bowel with a flap of tissue from the rectum.
This has a lower success rate than a fistulotomy, but avoids the need to cut the anal sphincter muscles.
LIFT Procedure
The ligation of the intersphincteric fistula tract (LIFT) procedure is a treatment for fistulas that pass through the anal sphincter muscles, where a fistulotomy would be too risky.(High fistulas) During the treatment, a cut is made in the skin near the anus between the sphincter muscles and the sphincter muscles are moved apart.
The fistula tract is identified and scraped out. The tract is then divided between two sutures and the initial cut is closed. This is a relatively new technique and has promising results.
Risks Of Anal Fistula Surgery
Like any type of treatment, treatment for anal fistulas carries a number of risks.
The main risks are:
- Infection – this may require a course of antibiotics
Recurrence – the fistula can sometimes recur despite surgery - Bowel Incontinence – this is a potential risk with most types of anal fistula treatment, although severe incontinence is rare and every effort will be made to prevent it.
- Immunosuppression – The risk of perianal abscesses is heightened in individuals with specific medical conditions or those taking immunosuppressive medications, such as those prescribed for HIV/AIDS or following organ transplantation, which can suppress the immune system.
Conclusion On Anal Fistulas And Perianal Abscess Treatment In Singapore
We have explored the topic of perianal abscesses, shedding light on their causes, symptoms, diagnosis, and treatment options. We have discussed the impact of perianal abscesses on daily life, the importance of timely medical intervention, and the significance of understanding long-term care for managing complications like anal fistulas.
If you suspect you have a perianal abscess or are experiencing related symptoms, don’t hesitate to seek medical help. Book a consultation with our colorectal surgeon,Dr Leong, who can provide personalised advice and tailored treatment options.
Remember, seeking professional medical assistance is crucial for accurate diagnosis, proper management, and preventing complications associated with perianal abscesses. Take control of your health and embark on the path to effective treatment and improved well-being.
Frequently Asked Questions About Anal Fistulas And Perianal Abscess Removal In Singapore
How Common Are Anal Fistulas?
How Do I Prepare For Anal Fistula Surgery?
Preparing for anal fistula surgery can be a daunting task, but it is essential to follow your surgeon’s specific pre-operative instructions to ensure a smooth and successful surgery. These instructions may include fasting for a certain period before the surgery.
It is also crucial to discuss any medications you are currently taking with your healthcare provider to determine if any adjustments are necessary. In some cases, you may be asked to undergo bowel preparation, which involves cleansing your bowels with laxatives or enemas before the surgery.
How Long Does The Surgery Typically Take?
The duration of surgical procedures for treating anal fistulas varies depending on factors like the type of procedure, complexity of the case, and individual patient factors. A fistulotomy typically takes about 15 minutes to an hour, while seton techniques and LIFT procedures may take around 15 to 30 minutes to 1 hour.
The advancement flap procedure is usually longer, ranging from 30 minutes to 1-2 hours. However, these are approximate timeframes, and actual surgical times can vary. Your surgeon will provide a more precise estimate based on your situation, considering factors like anaesthesia and pre-operative preparations.
What Kind Of Follow-Up Care Is Required After Anal Fistula Surgery?
If you have recently undergone anal fistula surgery, it is important to understand that follow-up care is crucial for a successful and safe recovery. Your healthcare provider may give you specific instructions for wound care and hygiene to prevent infection.
In addition, pain management medications may be prescribed to alleviate discomfort. Following a high-fiber diet may also be recommended to promote healing and reduce the risk of recurrence. It is important to attend all scheduled follow-up appointments with your healthcare provider to monitor your progress and assess any potential complications.
Will I Need To Have A Follow-Up Surgery Or Additional Procedures?
Some patients may experience complications or recurrence of the fistula, which may require further intervention. Regular follow-up appointments will help your doctor assess your healing progress and determine if any additional treatments are necessary.
Are Perianal Abscesses Contagious?
Can Perianal Abscesses Recur After Treatment?
What Are The Potential Complications Of Untreated Perianal Abscesses?
Are There Any Lifestyle Changes That Can Help Prevent Perianal Abscesses?
Although perianal abscesses may occasionally appear without a specific cause, implementing certain lifestyle modifications can help decrease the likelihood of their development.
Adhering to proper hygiene practices, for instance, regularly cleansing the perianal area with mild soap and warm water, can effectively reduce bacterial growth and promote cleanliness.
Avoiding trauma to the anal area, practising safe sexual practices, and managing underlying conditions such as inflammatory bowel disease or diabetes can also contribute to prevention.
Can Perianal Abscesses Be Treated With Home Remedies?
Is There A Link Between Perianal Abscesses And Sexually Transmitted Infections?
Can Perianal Abscesses Be Prevented Through Proper Hygiene Practices?
Are There Any Dietary Recommendations For Individuals With Perianal Abscesses?
While no specific dietary recommendations exist for individuals with perianal abscesses, maintaining a healthy and balanced diet generally benefits overall well-being and immune system support. It is recommended to incorporate a nutritionally balanced diet consisting of ample fruits, vegetables, whole grains, and lean proteins.
Additionally, maintaining hydration by consuming an adequate amount of water is vital for overall well-being. However, consulting with a healthcare professional for personalised dietary recommendations based on individual needs and underlying medical conditions is always advisable.
About Dr QM Leong
Colorectal & Hernia Surgeon in Singapore
Dr Leong is a general and colorectal surgeon in Singapore who graduated from the University of London in 2000. He obtained his membership to the Royal College of Surgeons of Edinburgh in 2003 and started working in Tan Tock Seng Hospital in 2003. He started his Advanced Specialist Training in 2005 and passed his fellowship exams in 2008. Dr Leong was awarded the prestigious MOH HMDP scholarship to train under Prof Kim Seon Hahn in Korea University for Laparoscopic and Robotic colorectal surgery in 2010.
Dr Leong is amongst a handful of hernia and colorectal surgeons in Singapore who practice Single Incision Laparoscopic surgery. This is a technical and complex procedure that is minimally invasive, speeds up recovery, and confers excellent cosmetic results. Dr Leong also routinely trains basic and advanced specialist trainees in laparoscopic surgery, and regularly proctors consultant surgeons in complex colorectal cases.
Beyond laparoscopic surgery, Dr Leong also performs a repertoire of minimally invasive General Surgery procedures. He is also an experienced endoscopist with more than 10000 procedures, performing diagnostic and therapeutic scopes for elective and emergency surgical conditions. He performs direct access colonoscopies and oesophago-gastro-duodenoscopy for patients and will strive to perform the procedures on the same day if possible for patients’ convenience.

Insurance
Our surgery is on the panel of most of the major insurance companies and if you are covered by corporate insurance, you may be entitled to a cashless visit to our clinic.
Get In Touch
Corporate Insurance Partners











Personal Insurance Partners







